| Died 15th August 1977
- |
| released 1st
December 1979 |
For many years, the relatives
of patients on the intensive ward have been left to their own devices and
neglected.
Information of the greatest import (diagnosis, complications, progress
or even death itself) have been (and are still) hurriedly given, unsupportable
briefly, often whilst standing in the corridor next to the intensive ward.
This behaviour results from an unwillingness to recognize and understand
what elements make up the reality and the experience of relatives
of patients on the intensive ward:
| |
The
relatives often suffer more about the unknown fate than the
patient himself. |
| |
Relatives have
an enormous need for information about the condition, therapeutic
measures and prognosis, which can only occasionally be fully satisfied. |
| |
Information
is usually given in a great rush by various members of the treatment
team. |
| |
Misunderstandings
or contradictory statements from the treatment team lead to anxiety,
uncertainty, suspicion and aggression. |
| |
As a result of
misrepresentation of intensive medicine by the media, the team member who
gives information is the one who is regarded as the "bearer of bad tidings"
on whom are heaped anxieties, anger, bad temper and aggression. |
| |
When a close
relative is receiving treatment in an intensive ward, not only the patient
but also the relative suddenly finds himself in a critical phase of
life. |
| |
Premorbid disturbed
relationships within the family are suddenly sharply accentuated. |
Typical types of reactions
from relatives can be observed if the progress extends over a prolonged
period (F.G. Müller quoted by Hannich).
| Basic rules for the care
of relatives of patients on the intensive ward |
| 1. |
Basic
premise: presence - empathy - acceptance |
| 2. |
Reduce the shock
of the "initial confrontation"! |
| 3. |
Gentle, simple
and warm-hearted speech |
| 4. |
Give hope |
| 5. |
Use appropriate
setting for discussion (not corridor) |
| 6. |
Take the various
phases of reaction of the relatives into account (denial, overactivity,
resignation?) |
| 7. |
Watch for the
reactions within the family set-up |
| 8. |
Give similar
information to all relatives |
| 9. |
No contradictory
statements from various team members |
| 10. |
Attempt to integrate
family members into the treatment team |
|
These are of importance for
the treatment team:
Phase 1:
Relatives seek to deny
the initially unbearable diagnosis and avoid believing that the illness
exists.
Phase 2:
The relatives know that
the patient is extremely ill, or will die, but do not believe it and rush
off into various forms of excessive activity.
Phase 3:
Discouragement follows
overactivity. The relatives recognize the full gravity of the situation,
but hypersensitivity and suspicion arise in this stage.
Phase 4:
Hypersensitivity and
suspicion become the source of a multitude of difficult questions and
reactions: "Is everything possible being done? Why is the patient on the
respirator? Why are so many machines in use? I am not satisfied with the
sister/staff/doctor; I am not getting enough answers to my questions."
Phase 5:
This is characterized by
both rational and emotional resignation.
| top |
 |
|
Communication within
intensive medicine
Nowhere else has communication
such a high priority as on the intensive ward; it is a basic necessity
for life. However there is also no other area within medicine where so
many obstructions act against it:
| |
Organic
and spiritual effects, as well as the effects of the disease itself |
| |
Obstructions
to communication caused by therapy itself (sedation, intubation,
artificial respiration) |
| |
Disturbances
in the relationship between patient and staff |
| |
Speech barriers
(medical jargon, foreign patient) |
| |
Time pressure,
overwork and lack of training within the treatment team |
The major aims of communication
in intensive medicine are:
| |
Placing
orientation markers: this means informing the patient of time and place,
about the objectives and the probable length of the treatment, and the
name and functions of the various members of the treatment team |
| |
Reconstruction
of the patient's feeling of self-worth. Its destruction is a hall-mark
of the reality of the patient on intensive treatment |
| |
Minimize anxieties:
those that predominate are those of separation, loss, suffering and the
future |
| |
Offers for
contact: being there, offering contact and projecting security, giving
and being aware of non-verbal attempts at contact |
| |
Give hope;
never ignore the "principle of hope"; this must be brought in even in the
most serious situations |
Even in situations where
there is no other solution, communication fulfils the function of "being
present as the other goes down" and then becomes the most important form
of care in intensive medicine.
The cardinal sins of communication
in the intensive ward (and not only there) are all those verbal and non-verbal
remarks and forms of behaviour which increase the feeling of abandonment
and anonymity of the patient, which increase his already disturbed feelings
of self-worth, which make him uncertain, which induce additional anxiety
and imply disinterest in what becomes of him.
Successful communication
on the intensive ward depends to an inordinate degree on the ability to
consciously communicate the 4 messages of speech (information, relationship,
self-revelation and appeal). Here the aspects of relationship (how we communicate
something to others) are more important that those of content (what we
share with others). Communication is one of the basic needs of mankind
and the desire for it is especially marked in these extreme situations.
Communications can take on the function of a "final anchor", on which everything
depends, and which holds everything fast.
The desire for communication
on the part of the patient on the intensive ward does not include only
information about the actual situation and the future eventualities. Since
life itself is threatened on the intensive ward, and death is an immediate
reality, there is a desire to review the events of past life, if not to
judge but to consider. These reflections about the life history are an
important mechanism for coping with the acute situation and should involve
the treatment team, each of them ought to possess the ability for active
listening. The manner in which the patient presents, in these reflections,
the things that he, helpless and dependent as he is now, was able to do
only a short while ago, is sometimes rather touching. This must be seen
as an attempt to stabilize his threatened feelings of self-worth.
An inexperienced person can
easily underestimate how much the seriously ill patient, who apparently
is not able to communicate, can in fact receive and register. It therefore
makes sense to continue to approach the patient with verbal and non-verbal
signs, even if the patient shows no obvious reactions. There is much evidence
to show that even in this situation the flow of communication is not one-sided,
but that it is also "received".
There are five methods
of communicating between the patient and the treatment team:
| Words |
|
Writing |
|
Mimic |
|
Skin contact |
|
Symbols |
If there is no handicap to communication,
it occurs over 10 communication channels. The following series of figures
show which combinations of disturbances are especially likely to arise
on the intensive ward and how the patient can be contacted nevertheless.
[IMAGES]
1. Patient has no handicap
to communication, 2. He is unable to speak, 3.
Patient is intubated and hard of hearing, 4. Mimic, 5. Patient is intubated
and has facial injury, 6. Patient is intubated and can understand neither
speech nor writing (foreigner), 7. Patient is intubated and paralyzed,
8. Patient is intubated and is blind, 9. Skin contact, 10. Patient is intubated
and unconscious
Writing is of particular
importance to the patient who can no longer use speech (due for example
to intubation). Felt-tipped pens (rather than pencils) and paper or blackboard
and chalk can be utilized. Studies have shown that this form of communication
requires a relatively large amount of time (on average 5-9 minutes) from
the moment that the desire to communicate is expressed to the determination
of what has been written. This includes finding and providing materials
and allowing time for writing. Communication boards which include recurring
patient needs, and can be touched to produce the words "yes" or "no", result
in a much better appreciation of requirements. Even patients who are unable
to speak or move can give, for example, eye signals which at least give
a positive or negative answer, for example, blinking = yes, or eyes closed
for a longer period = no. Obviously in these situations only closed questions
can be asked.
Examples of patients on
an intensive ward, most of whom were intubated or on the respirator:
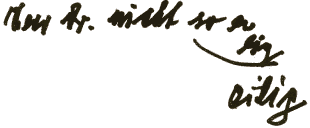 |
Doctor, sir,
not so quickly. |
|
|
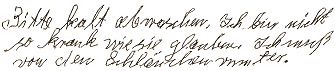 |
Please wash
with cold water. I am not as ill as you think. I must get off of the tube. |
|
|
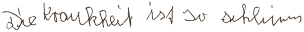 |
The illness
is so awful. |
|
|
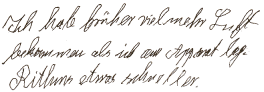 |
I got more
air previously, when I was on the machine. Rhythm somewhat faster. |
|
|
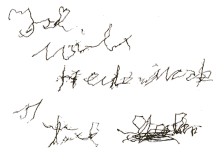 |
I want to
die at last today. |
|
|
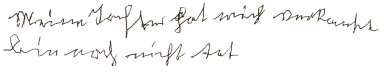 |
My daughter
has sold me, but I'm not dead yet. |
|
|
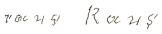 |
Get out, get
out. |
|
|
 |
A cardiac
catheter was inserted from the my neck into the heart when I was on the
medical ward in May and June. I am also allergic to plaster and injections,
and had to go into the skin department at Essen. Temporarily. It is so
rattly in my neck and lungs, that it sounds as if something is there. |
|
|
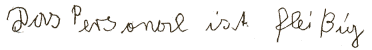 |
The staff
are busy. |
There is a series of simple
rules which should govern discussions between doctors and patients on the
intensive ward.
Initial ground rule:
Use the patient's name when speaking to him, and introduce yourself to
him by name.
G. Hensel, previously a patient
on an intensive ward, writes: "Every word which is directed to the patient
on the intensive ward, every single word, however simple, helps him to
escape from the feeling of loneliness and neglect. There is no other word
that the patient likes hearing as much as his own name. Although nobody
really wants to admit it, everybody is blessed to a certain extent by hearing
his name. If his name is forgotten, mistaken or mispronounced, he experiences
this as a body-blow. This feeling understandably becomes even stronger
in the extremely exceptional situation on the intensive ward. The person
who is spoken to by name is no longer anonymous, he is no longer a number;
he is being treated as a person in his own right, he no longer has to remain
in anxiety-creating anonymity. A further aspect is that it is particularly
helpless patients who dread being mistaken for another; one of the most
basic anxieties is that of being mistaken for another."
If the patient is addressed
by his own name, he takes this as a signal that he is recognized as a person
with his own particular problems in a specific situation. Doctors and staff
can also take steps to break down anonymity and background anxieties by
clearly naming themselves and describing their function. Orientation is
made particularly difficult for this patient by the system of intensive
care with the high numbers of staff of various functions, shifts and a
rapid change over in the treatment team. If the patient is to stay for
a prolonged period on the intensive ward, it is very important that he
is able to name at least one doctor and one member of the nursing staff
as a person of reference.
Second ground rule:
Offer help with orientation as soon as possible
Time should be taken to inform
the patient about the place, the time of day and the objectives of care
in the intensive ward, as well as checking that there are no misunderstandings.
There is nowhere else where the patient is so likely to be unsure of the
time as on an intensive ward. Much restlessness due to the confusion of
day-time and night-time can be prevented by this simple information. The
unreasonable rule that patients should not take any "personal belongings"
on to the intensive ward is still widely practiced, and whether or not
the patient needs his watch is overlooked.
The objective of the care
in the intensive ward should be explained as simply as possible. It is
sufficient to use terms such as "the illness can be controlled better",
"in order to make you better as rapidly as possible", "to deal with the
illness as well as possible " etc. The patient also should be informed
about the likely duration of the therapy. If this cannot be stated with
any degree of certainty, it can still be useful to tell the patient that
his stay will be "as short as possible".
It is also very important
to tell the patient that his relatives have been informed, and what has
been said. Uncertainty about this is particularly stressful and unsettling.
Telling him that "we have phoned your wife and told her that you are doing
well" is calming in two senses.
Third ground rule:
simple and comprehensible language
This is particularly important
on the intensive ward where the ability of the patient to register is limited
by the particular severity of his illness and by therapeutic measures.
Every word takes on a weight of its own, and every incomprehensible or
misunderstood statement can induce intense anxiety. It should be obvious
that during a ward round on the intensive ward, the patient should only
be spoken to and not about. Discussing the patient, additionally
in medical jargon, increases his feeling of isolation, releases further
anxieties and can be misinterpreted as signifying that the treatment team
is uncertain.
Although it is not possible
to prevent discussions about the patient, he should always have a simple
explanation about the subject matter under discussion; for example: "We
are not being secretive but are thinking how we can best organize your
treatment".
Fourth ground rule:
explain what is happening and what is planned
Even the smallest procedure
(for example taking blood, central venous pressure measurement) should
be explained to the patient in general terms if he has not undergone it
before. This reduces misunderstandings and erroneous conclusions and prevents
avoidable anxiety. One of the cardinal sins of communication is that a
patient undergoes an investigation, of which the objective and possible
meaning is not explained beforehand.
Fifth ground rule:
positive language
Anxiety, resignation and
depression are characteristic of the attitude of the patient on the intensive
ward. Every piece of information that can be formulated as a "positive
news" or "good news" is particularly important. The patient does not only
want to see but also to hear that he is out of the most severe
danger zone. This information does not have to be detailed, but is even
more convincing if it can be simply and clearly formulated:
"The operation went well",
"The X-ray didn't show anything
bad",
"I am very satisfied with
the progress you are making."
Illustrative (picture) language
is often more appropriate to describe the trend of the progress of an illness
than long-drawn out clinical findings. Phrases such as "land is in sight"
or "you will soon be able to fell trees again, even if at first only seedlings"
are often more reassuring of progress than information about haemodynamic
or biochemical parameters.
As in oncology, it is very
important to take so-called small problems of the patient on the
intensive wards very seriously, and to deal with them carefully. It is
these "small problems" which can be even more distressing than the major
medical problem. The psychological dynamics must be taken into account:
the patient who is aware that his comparatively small complaints are dealt
with as much care as the other medical problems, probably experiences his
situation as much less hopeless. Taking care of the small problems reduces
the pressure of the greater difficulties.
A patient, previously on
an intensive ward described this sort of event as follows. In the next
bed was an Italian who was unable to understand what was going on around
him. The single word which he continually repeated, although it was not
understood at first, was "graveyard". Everything that was happening to
him seemed to him to be a further step in the direction of the grave. Various
attempts to calm this extremely anxious patient failed. The solution of
this distressing situation occurred when a quick-witted nurse brought the
Italian his breakfast with the words "Not graveyard, but mangiare!", and
afterwards the surgeon enquired about the quality of this breakfast. "If
the doctor has no greater concerns than about how my breakfast tastes"
surmised the Italian, "then I cannot be so bad as I thought".
Sixth ground rule:
give hope
Everything should be done
to increase the hope of a patient on the intensive ward, where it is of
particular importance. This includes not only noticing small advances
in progress, but also informing the patient of them. It is equally
important not to show one's own concerns in the face of setbacks or unfavourable
progress. The patient needs a stable and safe and effective team, that
can be cheerful and even react with humor at appropriate times.
When the patient asks about
"the meaning of life" or "final things", or wishes to speak about life
and death, these subjects should not be avoided. When else should a person
start to think about those things which he has usually put aside during
a whole life-time, than when his life is extremely threatened? In these
situations, the doctors and staff are required more to listen actively
and to be present than to find answers to questions which often cannot
be answered anyway (see chapter on talking about God  ). ).
| Ground rules for carrying
out discussions with patients on the intensive ward |
| 1. |
Offer
opportunities for intensive contact! |
| 2. |
Use all
sorts of methods for communication (speech, written word, mimic, skin contact,
symbols) |
| 3. |
Offer help
with orientation |
| 4. |
Inform (place,
time, team, treatment) |
| 5. |
Do not induce
anxiety, instead make constant efforts to remove anxieties |
| 6. |
Simple, comprehensible,
positive language |
| 7. |
Speak to
the patient, not about him |
| 8. |
Give hope |
| 9. |
Support patients'
feelings of self-worth |
| 10. |
Do not avoid
discussions about life and death |
|
| top |
 |
|
Looking after the
relatives
The relatives are usually unprepared
to see a member of their family receiving treatment on the intensive ward,
and most of them show a shocked reaction. Their behaviour is emotional
to a large extent. It also depends on the quality of the relationship with
the sick person, and is influenced by the negative picture of intensive
medicine represented by the media.
Looking after the relatives
is part of the complete concept of treatment and should not be regarded
as an extra heavy load or duty. To care for relatives also passes care
onto the patient, as the crisis in which the patient finds himself is usually
also a crisis for the relatives. Carefully and adequately prepared relatives
can provide a source of strength to the patient, and its effectiveness
should not be underestimated. On the other hand, animosity to the treatment
team and the intensive ward on the part of the relatives can make therapy
very much more difficult. The ideal situation is one in which the relatives
have been successfully integrated (in the broad meaning of the word) into
the team.
The doctor, who is often
at the limit of his physical and emotional resources due to his work on
the intensive ward, repeatedly finds himself confronted with the apparently
insoluble duty of building bridges with a relative whom he might regard
as difficult or an additional load. In doing it, he is confronted with
the most varied reactions and forms of behaviour, including aggression,
grief, helplessness, insecurity, guilt, anxieties, blame and claims for
compensation. The doctor possibly finds himself regarded as an enemy resulting
from the picture projected of the intensive ward by the media. At other
times, relatives appear to have childish, naive, almost magical illusions
"that everything is possible if all of the resources of intensive care
are used" (Monika Dorfmüller). Perhaps they will also be hounded by
thoughts of publicity during a prolonged death, as for example Franco in
Spain or Tito in Yugoslavia, in which details of the prolonged death were
followed avidly.
Enormous difficulties can
arise in trying to manage discussions in such psychologically complex,
emotionally charged situations, and balancing the requirements of the patient,
the rights of the relatives as well as explaining the necessary medical
eventualities as plausibly as possible. The reason why so many discussions
with relatives are avoided or fail is that it is no longer possible to
find a common reality between the treatment team and the relatives.
Every discussion between
the treatment team and relatives needs to create the feeling of presence,
availability, empathy and acceptance. The next step is to consequently
break down understandable anxiety and provide comforting information.
Relatives definitely expect an immediate involvement in their helplessness
and the situation in which they find themselves.
The initial step is to buffer
the shock of the first confrontation with the sick patient. The
relatives in fact "are those who are the most shocked, even more than the
patient himself. They are shocked by the amount of equipment, within which
it may even be difficult to find their sick relative" (B.F. Klapp). This
alarm can be reduced if the relatives are well informed before taking them
to the patient. The doctor should be present during this initial meeting,
amongst other things to be available to immediately answer questions which
arise. The discussion should be carried out in comforting, simple language,
which also always encourages hope.
It should be attempted to
keep all of the relatives informed at about the same level of information,
in order not to create mutual insecurity. Where there are many relatives,
it is useful to find a single, major discussion partner who can
ensure that comforting information is evenly and appropriately distributed
throughout the family to put their minds at rest. This does not have to
be the next-of-kin.
It is also important to determine
in which of the previously mentioned "phases" the relatives are situated,
in order to be able to understand their questions and behaviour, to tolerate
apparently irrational reactions, to recognize the significance of accusations
and aggressive behaviour, as well as preventing escalation of emotional
tension between the relatives and the treatment team. Whether the relatives
are to be regarded as "friend" or "foe" of the treatment team depends to
a very large extent on the treatment team itself.
| top |
 |
| previous page |
 |
| next page |
 |
|
|
Linus
Geisler: Doctor and patient - a partnership through dialogue
|
|
©
Pharma Verlag Frankfurt/Germany, 1991
|
|
URL
of this page: http://www.linus-geisler.de/dp/dp27_intensive_medicine.html
|
|