| The best way to convince |
| others is with the ears: |
| by listening to them. |
| Dean Rusk |
|
"Little Momo could listen
in a way that nobody else could. That's nothing unusual, some might say,
everybody can listen.
This is not true. There
are only a very few people who can really listen. And the way in which
Momo listened was absolutely unique.
Momo could listen so that
inarticulate folk suddenly came out with bright ideas. It wasn't anything
that she said or asked that brought such ideas out of the other person;
no, it wasn't that. She simply sat there and listened with full concentration,
completely involved. While she gazed at them with her huge dark eyes, others
felt unique ideas (which they had never guessed were there) suddenly surfacing
from deep within.
She could listen so well
that restless or undecided people suddenly realized exactly what they wanted.
The timid unexpectedly felt free and bold. Those who felt unlucky or depressed
exuded confidence and joy. And if somebody felt that something was missing
from his life, which had become meaningless (that he was only one of the
teeming masses; that he could not manage and would be discarded like a
broken jar) - then he would go and tell little Momo all about it. While
he spoke about it, it would become clear in some secret hidden way, that
he was basically mistaken; that there was only one of him, that he was
unique, and because of that, he was important to the world.
How Momo could listen!"
Active and trained listening
is the most important ability that the doctor should use in discussions
with patients. As it is more difficult to listen than to speak, listening
is also the more difficult component of discussion. A specific characteristic
of the good doctor is that he has a good listening style.
Active listening means a
"ready-to-receive" attitude, or "attentive behaviour". This does not only
involve taking in what is said, but also developing an ear for the background,
and what is not said, as well as the semi-tones or emphases.
There are 4 preconditions
associated with active listening:
| 1. |
Interest |
| 2. |
Readiness
to listen |
| 3. |
Ability
to listen |
| 4. |
To be completely
present
or "all there". |
Additionally, it is also
important that the person I am listening to, knows that I actually am listening
to him. This means that he should be given a signal that readiness
to listen is present. This can be achieved by the use of a non-verbal signal
(eye-contact, body posture, gesture) or with a verbal utterance which encourages
him, as well as by the use of complementary or explanatory statements or
questions. Active listening then also involves attentiveness, signaling
interest, receiving the message and assimilating the message.
Active listening is an active
component of discussion and has to be present. It complements speech. Both
of these factors are components of discussion, and neither can form dialogue
alone. The interlacing of speech and active listening builds up true discussion.
The development of every
dialogue is associated with an unhindered interplay of alternating speech
and listening. Interruption is an extreme reversal of active listening,
and a prime disturber of speech; it is basically the most damaging form
of inattention. Listening is an active form of silence; it is a wordless
expression of: "I have understood, I can appreciate what you would like
to say". Sometimes silence in the form of active listening is the only
form of speech which is appropriate.
Listening must be unmistakably
listening, and should not arouse the impression of partial uninvolvement
or disinterest. It is easy that this confusion arises, as the patient does
not often receive the honour of being listened to actively.
An example which shows how
little doctors have heard of active listening comes from Günter F.
Gross: "I recently told a group of a few doctors: 'My doctor is an exceptional
listener; I spent 5 minutes explaining something, and he did not interrupt
me a single time.' The doctors looked at each other and became more and
more light-hearted. One told me: 'We can appreciate that you gave him the
chance, at last, to completely switch off, to relax and to think about
his own problems in peace!' I still find myself wondering if that were
really true."
What effect does active or
("controlled") listening have on the person I am talking with? It releases
a whole series of positive factors. The other person feels that he is a
real person who is accepted along with his problems. He feels relieved
and reacts less emotionally. He himself can concentrate on what is most
important. He needs less time to express himself clearly and is more convinced
that the other is "present and thinking about him".
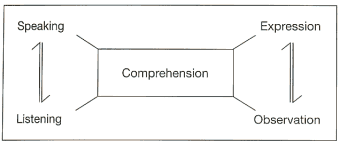
Comprehension is the
result of the interweaving of speaking, listening, expression and observation.
Mistakes in listening
have the following far-reaching consequences for patients:
| |
The
patient is not allowed to express himself |
| |
The patient cannot
utter his feelings |
| |
The patient feels
he is not taken seriously |
It must be said once again,
as it is of such basic importance: listening is more difficult than speaking.
It requires patience, concentration, discipline, analytical thought and
an awareness of semi-tones. There is an intense inner strain without a
corresponding outward activity. Active, analytical and discerning listening
is the highest step in an attentive attitude.
| top |
 |
|
Technique of "mirroring"
(reflection)
The technique of mirroring is
complementary to active listening, and an important supplement of the most
important of all interview techniques. Active listening and mirroring
together are the most intimately related and most productive elements of
every interview.
Carl Rogers and Reinhard
Tausch are the originators of the mirroring technique. However, even Sigmund
Freud said: "The doctor, like a mirror, should not show anything other
than what he is shown".
The principle of this reflection
is based on the fact that the doctor should give back to the patient whatever
he has heard and understood; that is, what he thinks he has understood.
This mirroring takes place in an empathetic setting with emotional warmth
(see chapter on empathy  ).
Here is an example: Patient: "I'm getting less and less enthusiastic about
life. He gets home so late every evening, and he is always tired. He doesn't
talk to me, or show any interest in me. I sometimes cry the next morning
and that helps a bit. I seem so empty. What can one do to change it all?" ).
Here is an example: Patient: "I'm getting less and less enthusiastic about
life. He gets home so late every evening, and he is always tired. He doesn't
talk to me, or show any interest in me. I sometimes cry the next morning
and that helps a bit. I seem so empty. What can one do to change it all?"
The doctor reflects: "Your
marriage seems to be hollow and meaningless at the present time. You feel
desperate and don't know how to react?"
This example shows how the
doctor uses the mirroring technique to play-back the present internal world
and the feelings of the patient in his own words, making her feel accepted
and understood.
Mirroring then involves putting
into words what the other cannot express easily. This initially imparts
a feeling of comprehension and acceptance. The most important effect lies
in the fact that mirroring helps the patient to gain more insight
into his own world of experience, his feelings, moods, presumptions,
behaviour, desires and goals. Mirroring encourages self-exploration
or self-study on the part of the patient. It leads the patient to "explore
his own emotional preconceptions, and judgements, his objectives and desires,
and becomes more clear about some of them, or attempts to become clearer"
(R. Tausch 1970).
This again makes it clear
that understanding discussion is a procedure in which diagnosis and therapy
are closely intertwined: in as far as I help my patient to gain more insight
into his feelings and conflicts, I create for him at the same time the
conditions under which can come to terms with them constructively. Mirroring
therefore is in the first place "the verbalization of emotional contents
of experience" (R. Tausch, 1970).
People react far more emotionally
and far less rationally than they would like to believe. As the head (mind)
finds arguments for ways of acting and behaving which come from the "heart"
(emotional world), we are strengthened in our belief that we are acting
rationally. Psychologists know well enough that most (and probably all)
of the "life decisions" of a person are taken emotionally and not rationally.
The philosopher Blaise Pascal once said: "The heart has reasons which are
not known to the mind." Many studies have shown that mirroring makes it
possible for constructive changes in personality, especially in cases of
psychoneurotic-tinged ways of behaving.
Mirroring affords the doctor
the opportunity to signal his understanding, and to put it into words without
the danger of interpretation, judgement or advice. It is also important
that he can express that he understands the patient without his
implying an immediate agreement with the contents. A comment which
starts: "I understand that you..." is usually unfavourable as this easily
releases the feeling of agreement with a certain attitude or way of behaviour
of the patient. This can be avoided if the doctor expresses his understanding
with: "Apparently the mess your son made of things left you so angry that
you felt you had to fetch him one...".
The decisive advantages
of mirroring are (mod. acc. W. Weber):
| |
The
patient feels that he is accepted and understood. |
| |
This means for
him that he receives partnership and tolerance. |
| |
It allows the
patient to get a grip on his internal experiences, his feelings, attitudes,
ways of behaviour, desires and objectives, and to manage them better. |
| |
For the doctor himself,
mirroring is a methodical and clear form for leading patient-centered interviews. |
| |
It allows the doctor to
choose the correct distancing or closeness to his patient. |
| |
Mirroring is the most impressive
way of signaling to the patient that the doctor is listening to him actively. |
| top |
 |
|
Techniques for interviewing
procedures in mirroring (reflection)
There are three discussion
techniques with which the doctor can mirror:
| 1. |
By
repeating
the words of the other. |
| 2. |
By repeating
what he has heard and understood in his own words; this technique
is called paraphrasing. |
| 3. |
By striving to
grasp the emotional contents of the experience of the patient in
words; this is called verbalization. |
Obviously all three methods
demand too much of the doctor at one time. However it is important to recognize
the possibilities, the value and the dangers of these three techniques.
The simplest of the three
is the repetition of the words (perhaps somewhat more briefly);
this does not require the doctor either to work on the formulation of his
words or take the trouble to go deeper into his understanding of the patient.
For example: Patient: "It was so horrible last night; I felt as if I was
going to suffocate. I never ever want to experience that again." Doctor:
"It was horrible for you last night." This response will do little more
than let the patient know that the doctor heard what he said, but it remains
in doubt whether he can really appreciate the fear of suffocating in such
an asthma attack. This is a technique which should only be used sparingly
as there is a very real danger that the patient experiences the doctor's
responses as "parroting".
Paraphrasing means
that the doctor replays what he has heard in his own words, at the same
time attempting to express what he believes he has understood. For example:
A patient who has had many
courses of chemotherapy says: "If it carries on like this, I can't take
any more." Doctor: "Do you want to finish the treatment then?" It is important
that the doctor has formulated his mirroring statement as a "floating
question ". He has given back what seems to him the most likely interpretation
of what the patient said, but would like to leave it completely free, and
available as a point of discussion, in case the patient meant something
else instead. In fact "what is meant" by what the patient says can be something
completely different i. e. "The treatment up to now has not helped much
", or "I can't cope unless you help me", or "I am at my wits' end" etc.
From this it can be seen that paraphrasing has the basic difficulty that
we can only give the patient one of the very many options of interpretation,
which is what we ourselves presume to be the most likely.
Verbalization is the
best method of getting in touch with the experience and feelings of the
patient. For example: The patient says: "I don't know if I can manage more
chemotherapy."
Doctor: "You are anxious
that it could get too much for you?" Here again the doctor has responded
with the method of the floating question, but this time focusing the discussion
on the likely predominant feeling of the patient, which is that
of anxiety. Here it is also clear that this statement permits many other
interpretations on the level of feelings. Probably the feeling of anxiety
is overshadowing true feelings of helplessness, despair, anger, hopelessness,
as well as aggression against the doctor. The method of verbalization includes
the major danger of misinterpreting the emotional experience, as well as
a tendency to judgement and interpretation.
W. Weber goes on from the
suggestions of Tausch to give the following concrete suggestions for the
procedures of discussion technique by mirroring:
| |
I
should mirror first and foremost the following contents.
| - |
emotional statements |
| - |
desires and objectives |
| - |
presumptions and emotional
judgements |
|
|
| |
technically
I should mirror:
| - |
all important
statements as soon as possible after they have been uttered |
| - |
briefly and concretely |
| - |
clearly and vividly |
| - |
what the patient is experiencing
and feeling in the "here and now" and |
| - |
make the attempt to work
out the meaning for the patient.
For example: "I wonder what
this means for you?" "I am trying to work out what is happening inside
you" |
| - |
use the term "you" ("you
have the feeling that...", "you would like that..."), rarely or never the
words "I", "We" or "one". |
| - |
try not to mirror mechanically,
as a façade or by echoing. |
|
|
If I am not sure whether
I have understood the patient, it is important that I mention it, for example,
by interjecting: "Is that right?", "I'm not completely sure if I have understood
you"? or "It seems as if I could understand you better if this point were
clearer".
As the doctor should use
his own words for replaying, it is especially important for verbalization
of emotional experiences that he deliberately broadens his own vocabulary.
Synonyms,
or words that tend to express the opposite meaning such as antonyms
should be studied. If for example the doctor picks up the statement of
the patient that he "feels alone", he could use the following synonyms
for reflection: "You have a marked feeling of loneliness", or " It seems
to you, that you have been abandoned". On the other hand, formulation with
antonyms would be: "You have the feeling that nobody is there for you",
or "You do not feel as though there is any loving concern for you at the
moment" etc.
Active listening and understanding
mirroring, especially with the verbalization of emotional experiences,
work together like cogs in a gear: this interaction of understanding listening
and expressing comprehension is the ideal engine for every understanding
discussion. The ability to listen actively and to express that which is
heard and understood so that the other feels that he is understood, extends
his view of himself and completes the higher levels of interview technique.
Typically this form of discussion does appear to be a work of art in its
effect but a "normal" discussion in its form. This is not new as is clearly
shown by the following lament of J.K. Lavater (1741-1801):
"If you can discover a person
who is peaceful,
without affectation
who, with presence of mind,
with true involvement,
can quietly listen to needs,
who does not interrupt,
who does not pose two questions at the same time,
who waits for the answer
and grasps it all,
who does not peer into the
future or past,
who does not fix you with
a studied look, and put you down,
who does not avoid your
gaze, looking upwards or downwards,
who is as prudent as he
is at ease, then -
then you will think that
you have found treasure in a field,
then you will think that
you have found a pearl".
| top |
 |
|
| Acceptance does not mean
much if |
| it does not include understanding. |
| C.R. Rogers |
Empathy should not be
confused with fellow-feeling, sympathy or "infectious feeling". It
also does not correspond to identification, from which the "as
if" characteristic is the most important difference. If the "as if"
is missing, there is identification but no longer empathy.
Sympathy is "an appraising
agreement with the feelings, ideas and the tastes of the other". As
with all judgmental forms of behaviour, it should not characterize discussions
between doctor and patient. Biermann-Ratjen underlines the importance of
the "as if" characteristic of empathy: "Empathy means to so completely
and so closely follow the experience of the other as if it were one's own,
but to never ever leave the "as if" state".
Empathy should also not be
confused with "being full of understanding in the sense of a humane attitude".
Obviously it is an ethically desirable form of behaviour to be "full of
understanding", but this is not an indispensable condition for interview
techniques. Although I do have to have the ability to feel for him in order
to be able to communicate about his problems, it is not necessary that
I am personally upset or involved. It can be said with some reserve that
involvement is more likely to impede free communication between doctor
and patient than facilitate it. Stated simply: a basic condition of doctor-patient
discussion is that the doctor is prepared to work towards understanding:
sympathy and compassion lie at another level of relationship. Empathy is
not only the ability to follow the feelings of the other. The emphasis
lies not so much on the term "feeling", but more on the ability of entering
into the world of experience of the patient. Rogers did not refer to
feelings, but more to the personal "perceived world" of his clients.
Doctors vary in their extent
of empathetic behaviour, as the ability to empathize depends on
certain conditions:
| |
The basic ethical
attitude of the doctor to his profession and his social involvement |
| |
His ability to
be moved emotionally, and his experience of coping with his own sensitivities |
| |
His ability to
perceive the quality of his relationships with patients and to influence
it (M. Geyer, 1985) |
There are two requirements
which can greatly impede the development of empathy: one is the
need for emotional neutrality and the other the need to dominate.
The desire to be empathetic is usually the reason for choosing medicine
as a profession. However most of the medical training is concerned with
understanding somatic disorders. Empathy is not required here. This may
also be stifled by defense mechanism against personal anxieties and guilt,
as well as experiences with pushy or clinging patients who cannot be managed
with an "empathetic approach". A need for emotional neutrality can develop
from this, which leads to an "ethically questionable distancing from the
human reality of the patient" (M. Geyer).
So the doctor also has to
know his own need for emotional neutrality and he has to integrate it deliberately
in his empathetic attitude. Only then he will be able to form both distance
and closeness to the patient according to his personality and to remain
susceptible to the patient's problems at long sight. The doctor who tries
to dominate the patient - mostly because of a lack of self-confidence
-, will misunderstand the patient's need for information and his attempts
to create a partnershiplike relation with the doctor and he will confuse
them with know-all manner and impeachment of the doctor's role. This conflict
makes it harder for him to behave empathetically (M. Geyer). Extensive
studies showed that the ability to develop empathy is facilitated by certain
features of the personality. These are: composure, good fellowship, the
ability to reflect and to be self-critical, general psychical stability
(M. Geyer).
Ultimately, the doctor should
be able to signal his empathy and appropriate understanding
towards the patient either directly or indirectly. The course of a discussion
which is characterized by involved understanding is often enough of an
indication of the doctor's empathy. If the patient finds that he can "get
through" with his problems or requests, and that these are interpreted
in the same way that he sees and experiences them, the doctor does not
necessarily have to reaffirm his understanding.
However, if the doctor gets
the impression that the patient is unsure that he has really been understood,
comprehension should be clearly affirmed. This can be done in two ways,
either directly by a verbal confirmation: "I can well understand, how you
felt at that moment...", "I know that this condition can be very unpleasant..."
The second possibility lies in indirectly implying that I am prepared to
involve myself and to understand by trying to describe his situation or
experience in my own words: "I think that you would like to tell me, that
you can't understand how it is that other people can laugh."
Empathy is the bridge which
leads from one's own reality into that of the other, and makes it possible
to determine a common reality. Empathy permits sorting out the various
problems that a patient has, not only in the abstract, but also to do something
about them. As a result one can understand that the otherwise apparently
inadequate reactions and behaviour of the of the patient are in fact perfectly
appropriate from his point of view.
Empathy is the key to understanding
the way in which a patient works through his experience of illness. It
is a precondition that doctors and patients really mean the same thing
when they discuss an illness. It is a prerequisite for a doctor-patient
relationship which is characterized by warmth and mutual acceptance, and
of a doctor being perceived as open and "real" (in other words he is what
he makes himself out to be). Empathy does not only mean that one has to
be prepared to put oneself into the patient's position for a short period,
but also to sense what the patient thinks of him (Dörner and Plog,
1980).
| top |
 |
| previous page |
 |
| next page |
 |
|
|
Linus
Geisler: Doctor and patient - a partnership through dialogue
|
|
©
Pharma Verlag Frankfurt/Germany, 1991
|
|
URL
of this page: http://www.linus-geisler.de/dp/dp04_listening.html
|
|